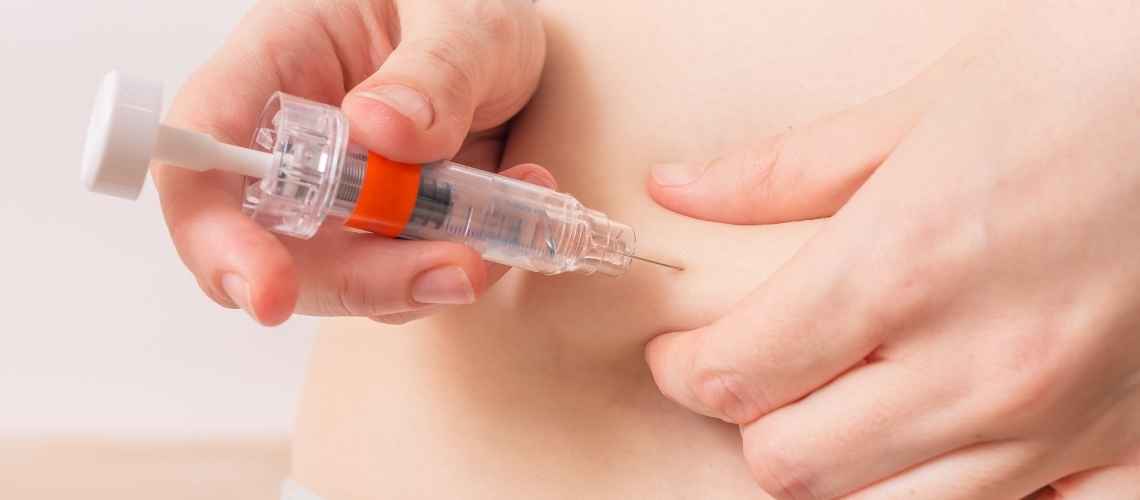
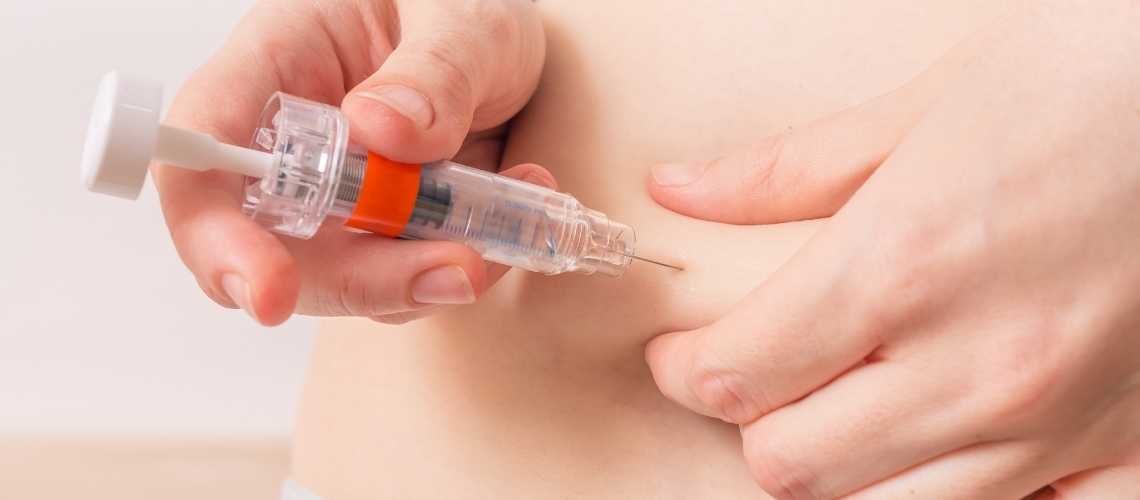
IVF and ICSI are both effective assisted reproductive technologies, but ICSI often shows higher fertilization rates, especially in cases of male factor infertility. Success depends on patient-specific conditions rather than one technique being universally superior.
IVF is typically recommended when sperm parameters are normal. In contrast, ICSI is preferred when sperm count, motility, or morphology are compromised, as it involves direct injection of a single sperm into the egg.
Pregnancy and live birth rates between IVF and ICSI are generally comparable in non-male factor cases. The main advantage of ICSI lies in overcoming severe sperm-related infertility that would otherwise prevent fertilization.
Choosing between IVF and ICSI requires medical evaluation of both partners. Fertility specialists consider age, ovarian reserve, sperm quality, and previous treatment outcomes before determining the most appropriate method.
What is IVF?
One of the more popular forms of assisted reproductive technology is IVF (ART). IVF helps sperm fertilize an egg and the fertilized egg implant in your uterus by combining medication and surgical treatments.
You first take medications to develop a number of your eggs and prepare them for fertilization. The doctor will then remove the eggs from your ovaries and combine them with sperm in a laboratory so that the sperm can fertilize the eggs.
After that, they insert one or more embryos (fertilized eggs) into your uterus. Pregnancy happens if one of the embryos implants in the lining of your uterus.
What is ICSI?
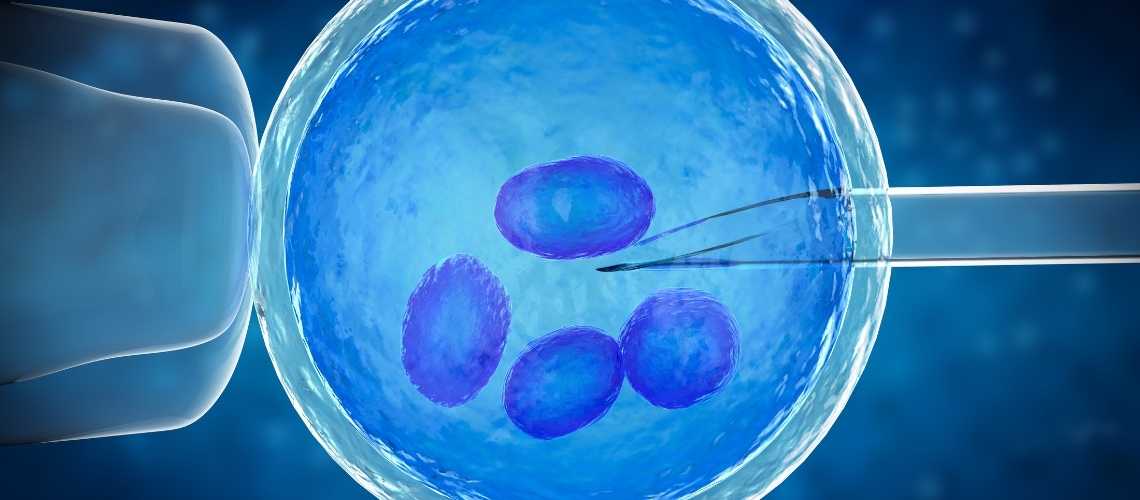
Even the most cutting-edge assisted conception techniques occasionally need a little additional support. An IVF treatment called intracytoplasmic sperm injection (ICSI) is used to break down obstacles that can impede a sperm cell from fertilizing an egg. It can dramatically boost the odds of getting pregnant for many people, especially those who are struggling with male infertility.
NHS estimates that 1 in 7 couples will experience difficulties while attempting to conceive. For about half of these couples, the issues are brought on by the male partner’s sperm. The term for this is male factor infertility. In certain situations, ICSI can be used in conjunction with IVF to enhance the chances of conceiving.
ICSI is not appropriate for all people undergoing fertility treatment; however, if male infertility is identified or there have been prior unsuccessful IVF attempts, ICSI may be suggested to improve the odds of success. (1)
What are the success rates of ICSI?
Although ICSI is incredibly efficient at promoting fertilization, it’s crucial to keep in mind that this is only one step in the IVF process. The success rate of IVF treatment as a whole continues to be correlated with the success rate in terms of pregnancy and live birth.
The success rates of individual IVFs using ICSI are not reported by the UK’s Human Fertilization and Embryology Authority (HFEA), the organization in charge of overseeing fertility clinics, because they are too close to those of conventional IVF.
Contrary to popular belief, there is no 100% success rate when sperm is directly injected into the egg. ICSI treatment results in successful fertilization in between 50 and 80 percent of instances, which is unquestionably very effective. The remainder is subject to further IVF and successful post-transfer implantation of the embryo into the uterine lining. (2)
Does ICSI improve embryo quality?
Modern medical practices offer solutions for infertility, with IVF being the most common method. IVF involves two main procedures: traditional fertilization in a petri dish and Intracytoplasmic Sperm Injection (ICSI), which is not an alternative but a component of the IVF process. Although not as widely used as traditional IVF, the success rate of ICSI is also high, but it cannot be said to improve embryo quality. In conventional IVF, the fertilization of eggs by sperm occurs in a laboratory setting. However, with ICSI, the embryologist selects a single sperm and uses it to fertilize the egg. The resulting embryo is then placed in the uterus of the female 5-6 days later
ICSI does not necessarily improve embryo quality directly, but it can help overcome male infertility issues that may affect embryo development. The quality of the embryo is influenced by several factors, including the quality of the eggs, the quality of the sperm used for fertilization, and the conditions in which the embryo is cultured.
ICSI helps ensure that fertilization occurs by directly injecting a single sperm into an egg, which may improve the chances of successful embryo development in cases of male factor infertility. However, the overall quality of the embryo still depends on other factors beyond the fertilization method used.
What is ICSI-IVF?
ICSI is done as part of IVF. Your IVF treatment won’t appear all that different from an IVF treatment without ICSI because ICSI is performed in a lab.
You will receive ovarian stimulating medicines, just like with standard IVF, and your doctor will keep an eye on things with blood tests and ultrasounds. A unique, ultrasound-guided needle will be used to extract the eggs from your ovaries if you have developed enough healthy follicles. (3)
What is the rate of success of ICSI-IVF?
50 to 80% of the eggs are fertilized during the ICSI process. You may assume that all eggs are fertilized by ICSI-IVF, but they are not. Fertilization is not always assured, even when a sperm is put into the egg.
Keep in mind that fertilization rates do not indicate the probability of a clinical pregnancy or live birth. A couple using IVF with ICSI has the same success rate as a couple using standard IVF once fertilization has taken place. (4)
When is ICSI recommended over IVF?
Intracytoplasmic Sperm Injection (ICSI) emerges as a tailored approach in specific scenarios within assisted reproductive technologies. Initially, for cases of male infertility, which include challenges like low sperm count, inadequate sperm motility, or unusual sperm shape, ICSI shines by offering a higher success rate. Moreover, when couples face the heartbreak of unsuccessful In Vitro Fertilization (IVF) cycles, specialists might pivot to ICSI. This shift aims to enhance fertilization prospects by directly injecting a single sperm into an egg.
Additionally, situations where egg retrieval yields a limited quantity underscore ICSI’s value. Here, the technique ensures each egg is given an opportunity to be fertilized, maximizing potential outcomes.
Male infertility factors:
- Low sperm count.
- Poor sperm motility.
- Abnormal sperm morphology.
Circumstances warranting a methodical shift:
- Previous IVF attempts resulting in non-fertilization.
Optimizing limited resources:
- Scenarios with a minimal number of eggs retrieved.
Furthermore, ICSI pairs effectively with Preimplantation Genetic Diagnosis (PGD). This compatibility is crucial for minimizing egg damage during the genetic testing process, which requires precision. Altogether, ICSI is not a blanket solution but a specialized intervention for overcoming certain fertility obstacles.
Source:
Martikainen, H., Tiitinen, A., Tomás, C., Tapanainen, J., Orava, M., Tuomivaara, L., … & Hovatta, O. (2001). One versus two embryo transfer after IVF and ICSI: a randomized study. Human Reproduction, 16(9), 1900-1903.